
The Complete Guide to Patient Engagement
The Importance of Patient Engagement
Introduction by HRS Chief Clinical Officer, Florence Kariuki, MHA, BSN, RN
Ten years ago, HRS’s Chairman and Co-Founder, Jarrett Bauer, set out to understand why his grandmother was revolving in and out of the hospital with recurrent congestive heart failure exacerbations. He investigated the causes for hospital readmissions, and found that the primary reason was basic—lack of continuity of care upon discharge, worsened by limited patient engagement in self-care. The system had failed in equipping Jarrett’s grandmother with an effective transitions of care infrastructure and in enabling her ability to understand and manage her condition appropriately.
Why I wanted to start HRS was because my grandmother was readmitted with heart failure... I looked into the reasons for readmission—non-compliance of medication, diet, lack of caregiver support, health literacy—and I thought wow, it’s all about engaging the patient to be proactive in their disease management. If you can give patients the tools to be successful, they’ll surprise you.

While the root cause was easily identifiable, the solution to the problem was much more complex. Although the healthcare industry has made great strides in implementing readmission reduction interventions, there remains much opportunity to continue addressing this issue.
Honing in on the opportunity to improve patient engagement in self care, it is evident that there isn’t a “one-size-fits-all” remedy—every patient requires unique resources, support, and interventions to optimally engage in their care and health outcomes. Patients may require a variety of tailored patient activation strategies to build their skills and confidence and consequently increase their engagement. These could include conducting effective teach-backs, use of medication reminders to improve adherence, enabling access to their medical records, convenient access to and communication with their provider, and ready-access to condition-specific educational resources, among others.
The challenge of limited patient engagement is a significant concern across the healthcare system given the growing evidence that patients who are least engaged in their care are more likely to have unmet medical needs and to delay care. Many patients are disconnected from their care due to lack of adequate knowledge and understanding of their medical conditions, as well limited access to the tools and resources that can help to improve their health literacy.
How can we improve patient engagement, and what are the benefits of doing so? What role can technology, and specifically telehealth and remote patient monitoring, play in improving patient engagement? This comprehensive guide will seek to answer these questions, and more, and offer information about the current state of patient engagement along with proven strategies to consider.
What is Patient Engagement?
Patient engagement describes the process of actively involving patients in their own healthcare. This includes sharing decision-making, self-management, and partnering with healthcare providers. Patient engagement is a key component of value-based healthcare, which focuses on improving the quality of care while reducing costs.
Patient engagement is an essential pillar for good health. As Dr. Farzad Mostashari, the former head of the Office of the National Coordinator for Health Information Technology once noted, “patient engagement is the blockbuster drug of the century.” When a patient is engaged, they are more likely to be proactive in their health management and to understand their condition. They are more likely to make the necessary behavior changes to positively impact their quality of life.

Patient Engagement
Patient engagement combines patient activation with interventions designed to increase activation and promote positive patient behavior, such as obtaining preventive care or exercising regularly.
A key part of patient engagement is patient activation. Patient activation is a measure of an individual’s understanding, competence, and willingness to participate in care decisions and processes. The ideal result of a patient engagement strategy or tool would be patient activation, plus care plan compliance. An engaged (and activated) patient takes the actions necessary to improve and/or manage their health.
Download our free infographic to learn more about incorporating telehealth and remote patient monitoring into your patient engagement strategy.
Patient Activation
A patient’s knowledge, skills, ability, and willingness to manage his or her own health and care.

An activated patient has the ability and commitment to:
- Self-manage illness or problems
- Engage in activities that reduce condition exacerbation or health decline
- Be involved in treatment and diagnostic choices
- Collaborate with providers and caregivers
- Select providers and provider organizations based on performance, quality, or their unique set of needs
- Navigate the healthcare system
The Benefits of an Effective Patient Engagement Strategy
A robust patient engagement strategy comes with many benefits. Two that are most notable are improved health outcomes and reduced cost of care.
Improved Health Outcomes
Patient engagement strategies improve outcomes by engaging patients in their own health. An engaged patient is more likely to take their medications as prescribed and consistently engage in condition self-management, resulting in fewer complications, unnecessary visits with their provider and fewer emergency admissions to the hospital.
When a patient is engaged in their own care during treatment, they will likely recover more quickly than their unengaged counterpart. They are more likely to be at lower risk for complications from uncontrolled symptoms.
Engaged patients are more likely to engage in preventative behaviors such as regular health checkups, immunizations, mammograms, nutritious eating, and STI/STD screenings. They are more likely to eat nutritious diets, exercise regularly, and avoid risky behaviors like smoking, using drugs, and drinking excessively. An engaged patient is more likely to identify a disease or diagnosis early, often resulting in avoidance of intense intervention or a grave prognosis, factors that are costly to the healthcare system and often, the patient and their family.
Patient engagement strategies enhance a patients’ understanding of their condition and treatment plan, boosting treatment success rates. They engage patients beyond the office visit by providing more provider touch points and opportunities for self-monitoring.
Research supports that patient engagement strategies improve patient care. One systematic review concluded that “patient engagement can inform patient and provider education and policies, as well as enhance service delivery and governance.”
Reduced Cost of Care
Healthcare organizations are under pressure to control costs and deliver value, especially as they assume more financial risk for population health management. Effective patient engagement solutions, like telehealth and remote patient monitoring, improve patient outcomes, which in turn, decrease readmission, emergency department utilization, and overall usage of the health system, resulting in reduced costs.
Engaged patients also free up hospital and provider resources by requiring less space, hospital time, and staff attention. This, in turn, reduces their total cost of care.
For more information on how telehealth and remote patient monitoring can be incorporated into your patient engagement strategy, download our free infographic.
The Challenge of Patient Engagement
Patients today, and the healthcare system as a whole, are complex. Many patients face challenges in obtaining, communicating, and understanding even basic health information.
In the United States, there are many barriers to optimal patient engagement and activation, including:
1. Communication and Language
For patient care to be effective, clear communication is crucial. Whether in the office setting, or via telehealth, if a patient and provider are not able to effectively communicate with each other the risk of poor outcomes is greater. Important information often goes in one ear, and out the other, simply because the patient does not understand, or does not feel empowered to ask questions.
Language challenges are a common barrier to communication. If a provider speaks one language, and the patient another, quality patient care can be very difficult. Conveying treatment options, medication changes, or a care plan, can be nearly impossible. In these scenarios, the risk is high of important information getting “lost in translation.”
Confusing or complex communication is another challenge, and one that ties back to health literacy, discussed below. If treatment plans, diagnoses, prognoses, and/or education do not meet the education level or literacy of the patient, it’s difficult to achieve good outcomes. It's important that providers incorporate robust patient education strategies into their care delivery models.
Addressing the Challenge
Shift from a focus on disease to a focus on health. Providers should ask patients, ‘What matters to you?.'” This question transforms the interaction from a conversation about clinical symptoms, problems and prescriptions to a discussion rooted in partnering together to achieve positive results.
Strategies to Improve Provider-Patient Communication
- Virtual visit and secure text messaging offerings
- Telehealth technology with multiple languages
- Translation services
- Incorporating the caregiver into communication
- Offer training on improving interpersonal communication (avoiding medical jargon, how to slow down, assuring understanding, asking the right questions, etc.)
- Emphasize nonverbal communication and body language
Health care is at the beginning of a dialogue with the world... As health care providers, we have to ask ourselves this question: What stories are we not hearing?Dr. Sachin H. Jain
President and CEO, SCAN Group and Health Plan
Communication tools can help improve patient engagement by providing on-demand patient access to their providers and caregivers. Download our free infographic to understand how virtual visits, language tools, and more, can help improve patient engagement.
2. Health Literacy
Health literacy, a patient’s ability to use, obtain, and process certain health information is a common barrier to patient engagement and activation. Current data suggests that about one third of American adults, or 89 million people, have insufficient health literacy skills. Without the tools and information to seek the care they need, these patients are twice as likely to report poor health outcomes.
A patient who is highly activated likely also has high health literacy. This person is by definition motivated to take control of their health, understands the steps to doing so, and has the ability to obtain the resources they need to effectively manage their condition.
Conversely, patients with low health literacy may recognize the importance of taking control of their own health but are unable to take the steps to do so due to insufficient understanding and knowledge.
Addressing the Challenge
To improve health literacy, providers need to meet patients where they are, and deliver care and patient education that meets a patient’s health literacy level. Using a patient health literacy assessment is a great first step, as is delivering patient education at about a fifth-grade reading level, or even in simpler language.
Understanding the patient’s baseline knowledge and what they already know about their condition allows the provider and patient to work together to create meaningful goals. When incorporating new tools into the patient's care plans, like telehealth, it's important to value the importance of patient education. This ensures patient's are set up for success.
Strategies to Improve Health Literacy
- Custom condition-specific educational videos
- Teach back quizzes
- Provide education in patient preferred formats (demonstrations, graphics, brochures, videos, one-on-one teaching, checklists etc.)
- Share appointment notes
- Learn what the patient knows, correct misinformation
- Include family members and caregivers
- Help the patient understand symptom trends
To understand how providers are leveraging these strategies with telehealth tools to improve education, download our free infographic.
3. Social Determinants of Health
The social determinants of health are “conditions in the environments in which people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks.”
These factors can hinder patients from obtaining good health outcomes. Often, the social determinants of health get in the way of a patient’s self-management plan. For example, a patient who does not have electricity, will not be able to charge their remote patient monitoring equipment. A patient who lives in a food desert and is food insecure will not be able to adhere to taking their medications on a full stomach. A patient who lives far from a healthcare facility, will not be able to access the services they need to achieve good health.
Addressing the Challenge
Healthcare providers must consider the social determinants of health before and during the delivery of patient care. Does the person have a strong social network, access to healthy food, a plan for medication management? Understanding the patient’s lived environment can help the provider customize the care plan to each patient’s unique needs.
Strategies to Address the Social Determinants of Health:
- Leverage SDOH screenings
- Prescribe affordable food options
- Connect patients with food and affordable housing options through partnerships
- Offer medical transportation
- Provide alternatives to in person care with telehealth
- Combat social isolation
Many healthcare organizations have also turned to telehealth to help address these challenges. It is beneficial to cater care plans according to a patient’s needs or limitations. Being cognizant about a patient’s social circumstances allows a provider to drive patient activation in a more realistic, empathetic way.
4. Patient Trust
The patient must trust their provider for patient activation to be possible. If a patient does not trust the healthcare organization or establishment as a whole, it is unlikely they will be able to obtain the level of patient activation necessary to improve outcomes.
Lacking patient trust stems from limited cultural competency, and the history some populations, for example Black and Hispanic populations have with the healthcare ecosystem.
Addressing the Challenge
Valuing cultural competency is the first step. Cultural competency is the openness and willingness to learn from patients—to allow them to be in the driver's seat of their healthcare. Defined, cultural competency is “the ability of systems to provide care to patients with diverse values, beliefs and behaviors, including the tailoring of health care delivery to meet patients' social, cultural and linguistic needs.”
When providers are able to deliver culturally competent care, they can build more trust with their patient. This results in an activated patient who is open to partnering with their provider to reach their healthcare goals.
Strategies to Establish Patient Trust
- Focus on empathy and body language
- Provide access to the patient portal to involve patients in the healthcare process
- Offer culturally responsive patient care
- Create a non-judgmental environment and avoid “medical fat shaming” as a strategy to motivate behavior change
- Level with the patient—be transparent about treatment and prognosis
- Educate staff to be aware of bias
Patient Engagement Strategies
The COVID-19 pandemic put more emphasis on patient engagement than ever before. During the pandemic, the entire healthcare ecosystem changed how it interacts with patients, evolving how patients receive and how providers deliver care. Patients had to adapt to avoid infection, becoming more responsible for and involved in their health than ever before.
4 Key Trends Influencing Patient Engagement
- Patients today want to get more value from their interactions with their providers.
The industry as a whole is becoming more consumer-centric, the patient is in the driver's seat of their own health, and they know it. Patients are becoming more motivated to improve their own health and engage in their self-symptom management. Now more than ever, healthcare organizations are placing more emphasis on patient experience, with a specific focus on experiences that improve loyalty, and provide more consistent care across the continuum.
- The prevalence of technology in our daily lives has risen exponentially, including availability of platforms that drive patient engagement.
At our fingertips we can communicate with anyone, anywhere. We have computers in our pockets. Patients expect 24/7 access to the internet of things (IoT) and they expect every experience to be digitally intuitive. Patients expect on-demand access to entertainment, food delivery, social media, and also, healthcare.
- Patients value education and health knowledge.
Providers agree that patient education does not translate automatically to patient engagement. Patients have an insatiable appetite for information, they want to understand everything there is to know about their health. Due to COVID-19, patients are more vigilant and interested in their health and that of their families. Providers understand that providing a handout to a patient at the end of an office visit does not automatically produce an informed patient-tailored, consistent, education is essential.
- The patient experience is center stage.
Healthcare is now a consumer-centric industry, and healthcare organizations have identified that healthcare consumers have many choices. Healthcare is evolving to be more focused on delivering personalized on-demand services, that are more focused on the patient experience, one that meets the patient “where they are”.
Patient engagement cuts across the continuum of care. It involves more than implementing a few new digital initiatives; instead, patient engagement calls for a complete rethinking of how providers connect with their patients, wherever they are. It requires a true commitment to changing patient behavior.
In today’s patient-centric industry, strategies that drive patient engagement are essential. And after all, information is power and engaged patients have better outcomes.
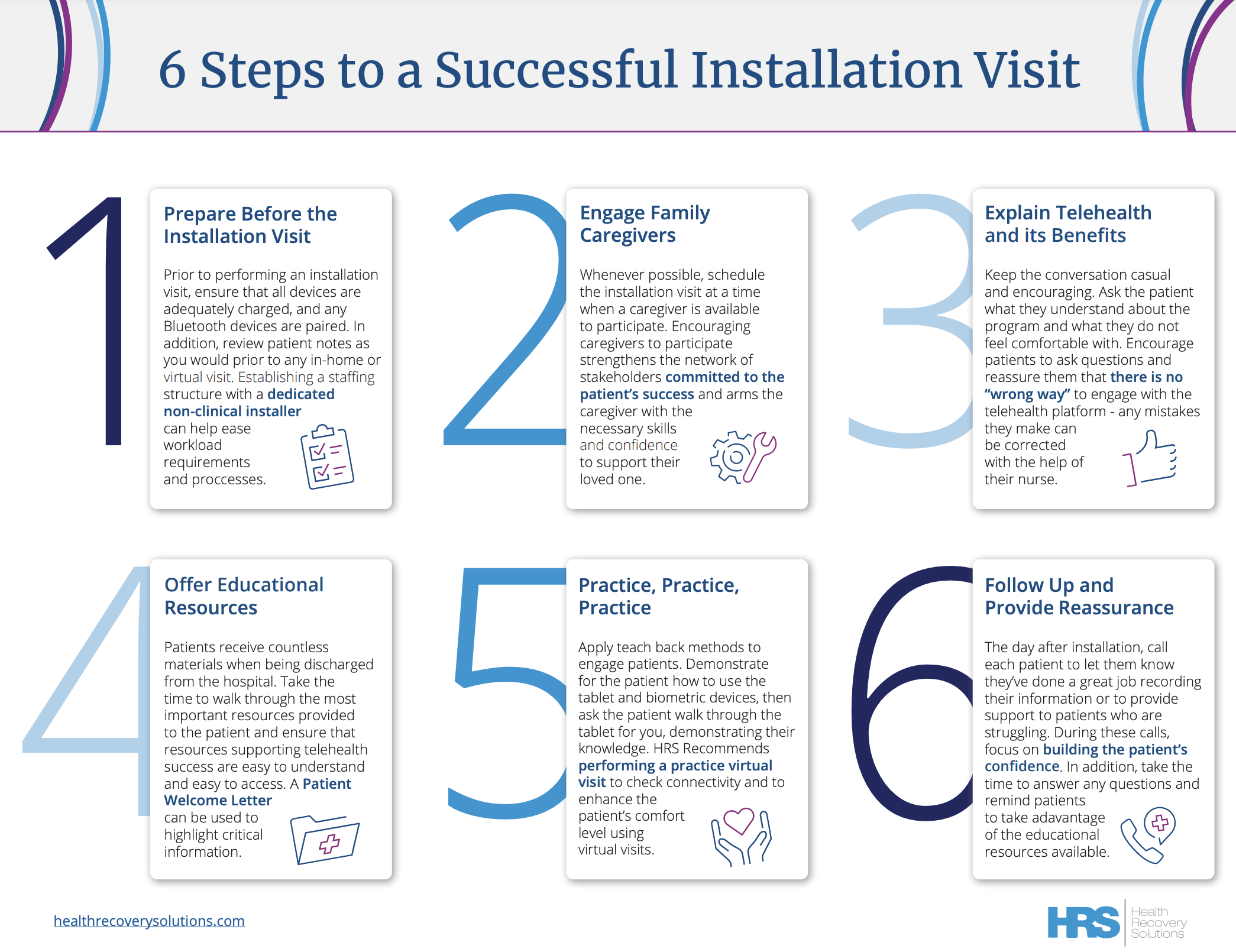
Launching RPM: 6 Steps to a Successful Installation Visit
Patient engagement, experience, and outcomes are largely dependent upon the patient’s introduction to telehealth and RPM. For many organizations, this introduction occurs during the installation visit. This quick reference guide covers the 6 steps for a successful visit.
The Shift to Digital Patient Engagement
Digital patient engagement programs enable providers to communicate with patients through digital channels that are convenient and accessible for the patient.
Examples of digital patient engagement strategies include:
- Using a mobile application to communicate with a healthcare provider or health coach
- Tracking activity via wearables
- Engaging in condition-specific education virtually
- Accessing on-demand symptom insights through a mobile application or tablet
- Using “smart” devices, such as smart inhalers, glucometers, thermometers, scales, etc.
- Texting patients
- Leveraging remote patient monitoring tools to track vitals, symptoms, medications, activity
For a digital patient engagement strategy to be successful, it should balance patient experience, patient access, and technology adoption.
To learn more about digital patient engagement strategies, download our free infographic on telehealth and patient engagement.
Patient experience and satisfaction
The patient experience should be at the center of any patient engagement or digital patient engagement strategy. When leveraging a digital engagement tool, for example, remote patient monitoring, the provider and patient must come together on a unique care plan. Every patient is different, so their digital patient engagement strategy should align with their unique needs.
Patient access
Digital patient engagement strategies inherently increase access to care by providing more touch points between the patient and provider, as well as more opportunities for the patient to engage in their own care.
More than ever, patients demand accessibility. Just as consumers expect convenience in entertainment, dining, travel, and other industries, patients expect the same accessibility to healthcare. Digital patient engagement strategies provide patients with access to their own healthcare data, information on their condition and providers, etc.
These tools offer mobile-first access to patients 24/7 at their own convenience, giving them the ability to complete routine tasks related to their medical care and health, using technology that is straightforward and convenient.
Adoption of technology
Technology is not “one size fits all” and every patient has their own place on the spectrum of technology literacy. Some are fluent in using technology day-to-day, while others are at a basic level of understanding. Regardless, all patients should be able to benefit from digital patient engagement tools. Finding the right solution for each patient, using clinical best practices, and keeping workflows simple ensures the success of technology. Telehealth education is crucial for patient success.
A robust digital patient engagement strategy is designed with the patient at the center, with the goal of improving outcomes, reducing cost, and decreasing barriers that patients experience in accessing health care.

Remote Patient Monitoring and Telehealth: 6 Key Features For Patient Engagement
When patients engage in their own care, outcomes improve and satisfaction increases. Costs are reduced and quality is improved. Wondering how to incorporate telehealth into your digital patient engagement strategy?
Download our infographic on 6 key telehealth and RPM features to improve patient engagement.
Related Resources


Transforming Trials into Triumphs: How RPM is Changing the Cancer Care Journey

