Virtual Care, Not Just RPM
Modern telehealth products have several different solutions and services to offer healthcare organizations. Some of these include remote patient monitoring (RPM), educational materials, communication tools, and medication and symptom tracking. Virtual care through video is only one communication feature, but probably the most critical of those features vendors can provide. Whether you are employed by an agency, health system, or nonprofit organization – executive, clinical, or nonclinical – you may be thinking:
How are virtual visits used? What is their purpose? Who is involved?
When should we be doing them, and how? What is the ROI?
Determining the answers to these questions for your organization will help define the role that virtual visits can play in improving patient care. Start by defining the problem that your organization faces, and focus on ensuring that you are leveraging virtual visits as a solution to that problem. When used correctly, virtual care through video will create an enhanced RPM experience, with another layer of engagement reinforcing connectivity and support.
Virtual Care Realities: Perceptions Are Shifting
When it comes to implementing the practice of virtual care, remember that change will not take place overnight, especially as clinician buy-in and appropriate staff are established. Making virtual visits part of the routine for patients and setting expectations on the patient and clinician side can take some time. A lot of home health agencies and health systems may see implementation take place across multiple systems and agency departments over a period of months or even years. Every organization is different in terms of staffing, structure, planning, and resources, so keep in mind that implementation is not a one-size-fits-all approach.
The Massachusetts General Hospital (MGH) research study documented evident support among multiple physicians for the practice of virtual care and scheduled virtual visits with patients (Roth ). The study highlights that due to an increasing availability of personal technology, patients and clinicians have the opportunity to leverage real-time virtual video to enhance telehealth services, past what traditional RPM has to offer, and with many real-time, and cost-effective benefits. Several authors are individuals who utilize video visits extensively in their own practice. Organizations can experience an initial period of resistance or lack of buy-in, but it is valuable to establish metrics that indicate success:
1. Thorough implementation and introduction to technology value and features (Organization-wide, executive and clinical staff)
-
-
Identify a telehealth coordinator or lead (this individual should also be a champion of virtual care)
-
Engrain the perceived value of virtual care by decision-makers into the day-to-day clinical staff
-
2. Proper hands-on virtual video training, testing, and question & answer
-
-
Notes: Multiple sessions are encouraged for clinical staff and appropriate groups. Attendees should not be afraid to ask questions.
-
3. Develop a sample virtual video visit script for the clinical monitoring staff conducting virtual care. Make sure it includes clear instructions on when virtual visits should be used and the content for those virtual visits.
4. Clear communication, brainstorming, and vision for virtual care in the telehealth program. Clinician comfort and ability to communicate effectively in performing the visit is just as important as the patient’s satisfaction and experience, in addition to, reduced travel time for clinicians and patients.
When starting out, it is important to consider WHO is conducting these virtual visits. This individual or team of individuals should be staff members that can provide clinical feedback to patients enrolled in telehealth services. We encourage organizations to think about how to leverage staff members more effectively. For instance, if you have a shortage of physical therapists, virtual visits may be an effective way to stretch your resources. At HRS, we realize how valuable the time is of the clinicians we work with on structuring and sustaining their telehealth programs. Adjusting to virtual care is not a small adjustment by any means, but technology and innovation are advancing patient care and clinical efficiencies every day.
Download the HRS Video Visits Guide
Best Practices for Virtual Visits
At Health Recovery Solutions, we have many best practices that we have learned from our virtual visit implementations.. With having an easy-to-access and user-friendly solution set up in the home like PatientConnect, you also have a fantastic virtual visit channel to provide the patient with clinical guidance and support. The patient is provided reassurance, access, and engagement with their care. It is also a great way to supplement or replace in-person visits in the patient home or trips to the clinic as appropriate.
Here, we will break down our Best Practices into (3) Categories:
Introducing Video Calls to Patients
We recommend introducing patients to the video calling feature as early in the process as possible. For some organizations, this could be while there is a tech or clinician in the patient’s home, for others it may take place at the hospital or clinic where the patient is receiving their telemonitoring equipment. With an early introduction, even patients unfamiliar or slightly reluctant to technology can get to know how the feature will work with close guidance and support from your staff members. It is also helpful to show them how they can be closely connected with their clinicians each day, right in the comfort of their own home during an important time of care and oversight.
Having a caregiver or family member available to participate in the installation and video visit training is also recommended. An early introduction to video calling will provide an opportunity for your telehealth team to meet the patient, and will make the process much more comfortable for the patient moving forward. Make sure to review with the patient any protocols you have about the hours of telemonitoring, who to contact after hours or if there is an emergency, and any other important information they should know about conducting virtual visits with your team.
Scheduling a Video Visit
Once the patient is into their telehealth enrollment, we recommend that additional video visits be scheduled in advance with the patient, and written down or documented. Scheduling can be done during an in-person visit or through a phone call or text message. One of the most important parts about this best practice is to let the patient know that the video visit should be treated just like a regular appointment. Make sure your clinicians follow the virtual visit script and protocol that you have created and are properly documenting the visit within the medical record.
With remote patient monitoring platforms like HRS, patients have access to text messaging tools, as well. Text messaging is a useful feature for non-urgent communication, in addition to an opportune method to remind patients about scheduled video visits. We recommend sending a text message the day before the visit to remind the patient. If you do not receive a response, it could also be helpful to call the patient on their land line or request they return your call in order to keep the appointment.
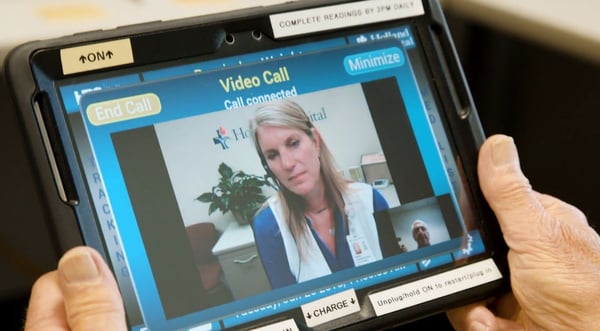 Image courtesy of Holland Hospital
Image courtesy of Holland Hospital
Patient-Requested or PRN Video Visits
A great way to ensure that patients are getting all their clinical questions and concerns addressed is to include a daily symptom survey question that asks whether the patient would like a nurse to call them that day. On the HRS platform, a high-risk alert can be added to ensure clinicians are notified when a patient indicates that would like to receive a call. In other circumstances, a vital sign out of normal parameters or a missed medication reminder might be a reason to do an unscheduled virtual visit with patients.
While clinicians do have the option to perform a standard voice call, video calling can be advantageous in that it allows the nurse to assess the patient’s physical well-being better and intervene as appropriate. Clinicians report being able to do medication training, assess wounds and other physical symptoms, view oxygen tubes, and many other clinical benefits in addition to being able to reduce patient anxiety. Unscheduled virtual visits allow clinicians to gather more information about each patient and prevent unnecessary ED visits, readmissions and save clinical time by providing clinical consults from wherever they are currently located.
Telehealth Etiquette, Some Webside Suggestions:
-
Consider eye contact with the patient and communicating clearly
-
Consider the video visit setting and surroundings
-
Be on time or a few minutes early to get settled and comfortable
-
Clarify your actions with the patient
-
Ask the patient for feedback
In reference to a blog on “Telehealth Etiquette” written by Michael Greiwe, MD, and published by OrthoLive, an orthopedic telehealth platform, he discusses that as telehealth usage continues to expand, clinicians must learn new workflows and best practices to implement new tools. If you can successfully develop these skills throughout your clinical staff, and work with teams like HRS, you can improve the patient and clinical experience, as well as ensure a successful telehealth program of service for years to come (Greiwe).
Benefits and Goals of Virtual Care
Through enhanced and real-time video conferencing, patients, clinicians, and all the individuals involved in the telehealth episode can communicate and interact quicker and easier. The patient can feel supported in their home by their caregiver or loved ones, especially those that choose to get involved with the technology. With their connected healthcare professional just a few steps away in their own home, it can be very comforting for the patient.
Mandy Roth, an innovations editor from HealthLeader Media, identifies a great deal of valuable findings from the staff at MGH throughout her article, and several notable findings in terms of patient feedback on virtual visits (Roth 2019):
-
79% of patients felt that finding a convenient time for a follow-up virtual video visit was easier than for a traditional office visit.
-
62% of patients reported the quality of virtual video visits was no different from that of office visits, and 21% thought virtual visits’ overall quality was better.
-
68% of patients rated virtual video visits a 9 or 10 on a 10-point scale. Patients who rated the visits lower experienced technical issues during their first use of the system. Those issues were usually resolved with technical assistance.
Ultimately, we want the main goal of the virtual visit experience to be augmenting in-person visits, broadening access to care, and providing user-friendly communication tools. Further, two hugely beneficial elements to virtual video visits are the ability to make interventions (ex: resolve medication discrepancies) and, improve care quality, reducing hospitalizations.
Senior study author Lee Schwam, MD reveals his personal opinions in regard to study they conducted at MGH. In a news release from Science Daily, Schwam said: "Our findings confirm what I felt in my gut, which is that what patients' value most is uninterrupted time with their doctor, and they put up with all the other challenges required to come see us” (Massachusetts General Hospital).
The Importance of Physician Collaboration
Within all disciplines of telehealth, it is vital to obtain buy-in from physicians and healthcare professionals who see the patient value in virtual care, and ultimately, the cost savings and efficiency it can provide. As the industry expands, so will the adoption of virtual care visits. The importance of physician collaboration is a key element to a lot of successful telehealth programs, as physicians can be directly involved in virtual care with clinicians, therapists, social workers, caregivers, and other professionals involved. Even if physicians are not the ones conducting the virtual visits, the information gained from the virtuals will allow for more accurate descriptions of patient status and which can lead to quick action on medication orders. Only through the collaboration of disciplines can we deliver the most effective care to patients.
How to Get Started
-
Have a discussion with your team and staff involved in video visits
-
Develop an implementation plan
-
Plan out training dates for relevant staff members and key stakeholders
-
-
Create necessary documentation for clinical staff to guide them through conducting virtual care
-
Sample Virtual Visit Script
-
Guidelines for when to perform virtual visits
-
-
-
Determine the location of video visits and where clinicians will be conducting calls in the office or in the field
-
Set up a virtual call space in your office for the best patient experience and environmental efficiency
-
Two Suggestions:
-
Central station that is one spot in the office with video and listening equipment
-
Self-Serve setup at clinical desk or station
-
-
-
Set up testing sessions to get comfortable with the technology and allow staff to participate directly
-
Roll out the virtual visits to a small cohort of patients first to get familiar with the technology
-
Apply lessons learned and keep expanding to new patients and new use cases!
Resources:
Greiwe, Michael. “Telehealth Etiquette – Conducting the Virtual Visit.” Telehealth Etiquette – Conducting the Virtual Visit, OrthoLive, 30 Mar. 2019, www.ortholive.com/blog/telehealth-etiquette-conducting-the-virtual-visit.
Massachusetts General Hospital. "Virtual video visits may improve patient convenience without sacrificing quality of care." ScienceDaily. ScienceDaily, 14 January 2019. <www.sciencedaily.com/releases/2019/01/190114130910.htm>.
“Virtual Care Perceptions Shift: Docs On Board, Patients Willing to Pay.” Edited by Mandy Roth, Virtual Care Perceptions Shift: Docs On Board, Patients Willing to Pay | HealthLeaders, 16 Jan. 2019, www.healthleadersmedia.com/innovation/virtual-care-perceptions-shift-docs-board-patients-willing-pay.
