With the advancement of new technologies, the field of telemedicine is continuously expanding, leading to a corresponding expansion in the applications of remote monitoring.Remote Patient Monitoring (RPM) has been a part of the healthcare landscape for years, allowing physicians and non-physician practitioners to monitor patients with chronic conditions from afar. Historically, RPM was used by home health agencies to reduce the number of in-home visits but when the COVID-19 pandemic hit, hospitals rushed to adopt RPM to keep patients safe and comfortable at home. Today, hospitals and health systems are expanding the use of RPM to provide a hospital-at-home level of care and support patients across the entire care continuum.
In 2021, the Centers for Medicare and Medicaid Services (CMS) approved the Medicare Physician Fee Schedule Final Rule, which provided new information on Remote Therapeutic Monitoring (RTM), differentiating RTM services from RPM. This approval expands the types of providers who can bill for remote monitoring services and broadens the scope of care provided.
In this blog post, we’ll explore the nuances between these two types of remote monitoring and what it means for providers and patients.
What is Remote Therapeutic Monitoring (RTM)?
Remote Therapeutic Monitoring (RTM) refers to outpatient rehabilitation therapy services that include monitoring how the musculoskeletal and respiratory systems are functioning, as well as therapy adherence and therapy response in patients.
With the establishment of the new RTM billing codes, which are a new class of general medicine codes, CMS created a clear differentiation between RTM and RPM.
RTM services can be provided by physical therapists (PTs), occupational therapists (OTs), and speech-language pathologists. These practitioners can order and bill for RTM codes without a physician or nurse practitioner, unlike RPM services.
Additionally, while RPM is focused on monitoring vital signs using devices that automatically record and transmit biometric data, RTM allows healthcare providers to monitor how patients move, use their muscles, and respond to the prescribed therapy through self-reported metrics. This broadens the scope of remote care to better support physical and occupational therapists.
What is Remote Patient Monitoring (RPM)?
Remote Patient Monitoring (RPM), also known as Remote Physiological Monitoring, focuses on monitoring a patient’s physiologic parameters such as weight, blood pressure, pulse oximetry, or respiratory flow rate outside of traditional healthcare settings using advanced remote monitoring devices. RPM is often used to monitor patients with chronic conditions such as hypertension, diabetes, COPD, and heart disease.
Unlike RTM, RPM billing codes are restricted to physicians and certain qualified non-physician practitioners (NPPs), such as physician assistants and nurse practitioners. The goal of RPM is to catch potential health issues before they become emergencies by encouraging patients to be more proactive in their health care plan.
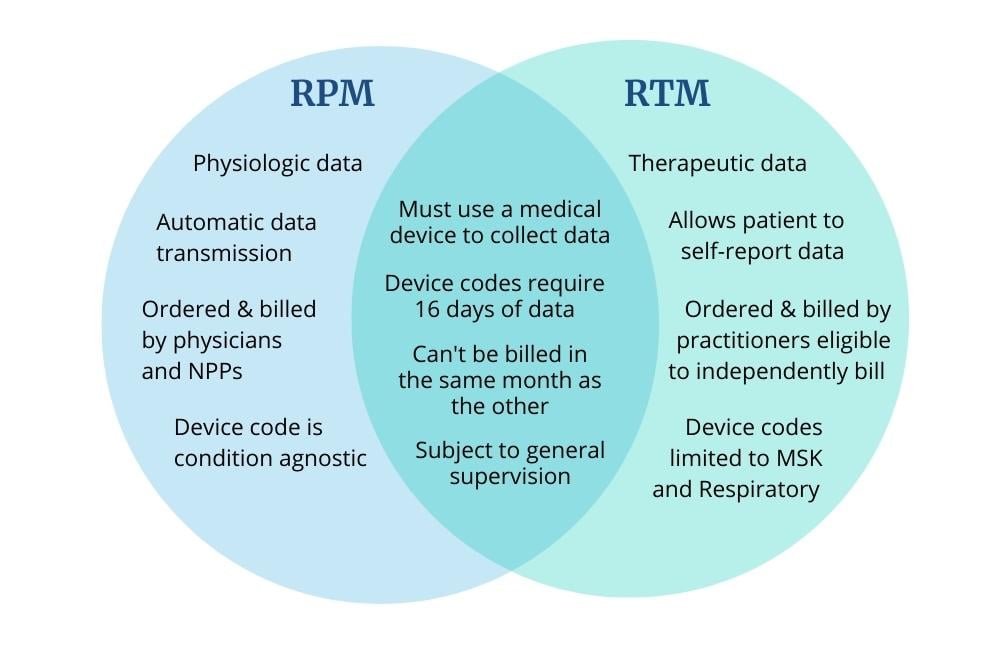
Key Similarities and Differences Between RTM and RPM
One of the most significant changes to remote monitoring with the introduction of RTM codes is the expansion of who can bill CMS for these services. While RPM was only available to physicians and certain non-physician practitioners, RTM codes have been expanded to include physical and occupational therapists, speech-language pathologists, physician assistants, nurse practitioners, clinical social workers and physiatrists. This broadens the range of care for these professionals, allowing them to monitor and adjust therapy programs based on objective data they capture remotely.
Another key difference between RTM and RPM is that patients can self-report data through an RTM program, but RPM programs require the automatic transmission of data through approved monitoring devices.
Remote Therapeutic Monitoring Reimbursement
RTM and RPM reimbursement criteria are similar in many ways, but there is one key difference to keep in mind:
RTM enables patients' self-reported data and digitally uploaded non-physiologic and therapeutic data. RPM, on the other hand, requires physiologic data that is automatically transmitted and not manually uploaded.
Beyond this requirement, billing for RTM is very similarly structured to RPM billing. RTM providers can receive reimbursement for educating patients about remote care-management platforms, monitoring a platform's alerts, direct messaging between patients and providers, and data collection—enabling feedback on pain levels, activity, and motion.
2023 Remote Therapeutic Monitoring CPT Codes: Cheat Sheet
In this cheat sheet, you’ll find a quick and easy guide to the five primary remote therapeutic monitoring CPT codes (RTM CPT codes) that are most relevant to your remote care program.
Expanding the Scope of Remote Monitoring
Remote monitoring has been a game changer for healthcare professionals seeking to provide better patient care at lower costs. With the introduction of RTM codes, healthcare providers can broaden the scope of remote monitoring, offering patients objective data on their therapy programs. Physical and occupational therapists, speech-language pathologists, physician assistants, nurse practitioners, clinical social workers and physiatrists. can now participate in remote monitoring, providing critical data that can lead to better patient outcomes. As remote monitoring continues to evolve, we can expect more nuanced solutions to emerge that help reduce costs and improve outcomes for patients with a broad range of conditions.
HRS supports healthcare providers navigating the telehealth reimbursement process. We've got you covered with in-house reimbursement specialists and automated reimbursement reporting.
Try the RTM Reimbursement Calculator
Curious to know what your reimbursement rate could be for providing remote therapeutic monitoring services? Use the RTM Reimbursement Calculator to view an estimate.