In times of uncertainty it is essential that individuals, especially those in the healthcare and health policy space, recognize the disparities that exist and focus on what can be done to address them. The Social Determinants of Health (SDoH) are the conditions and the environment in which people are born, live, learn, work, play, worship, and age, that affect a wide range of health risk and outcomes, as well as overall quality-of-life.
Within the Social Determinants of Health, there are five determinant areas that are used to categorize factors:
- Neighborhood and Built Environment
- Health and Healthcare
- Social and Community Context
- Education
- Economic Stability
Keeping these determinants in mind, the goal is to create environments that not only promote good health but also sustain it. To achieve this goal, healthcare workers should understand the area of health and healthcare specifically.
Determinant Key Area: Health and Healthcare
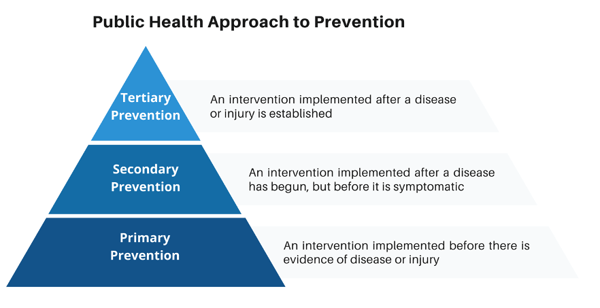
Improving access to healthcare, access to primary care, and health literacy are all current issues that need to be addressed to promote healthy lifestyles. These health-related behaviors are not the only factor when it comes to a healthy lifestyle, but they do have an impact on a person’s quality and length of life. Access to primary care is a key component in health promotion and primary prevention. Primary prevention can be defined as, “an action or behavior that does not allow disease or adverse events to occur” (Hensrud, 2000). Individuals with access to primary care work closely with a healthcare team to not only improve their health but identify ways in which they can avoid negative health outcomes, such as quitting smoking, getting immunizations or creating better eating habits.
It is not enough to just state that there are key areas to focus on within Health and Healthcare, there also needs to be initiatives to ensure individuals have access to these opportunities. Many of these initiatives do not only focus on one determinant area, which allows for a better opportunity to increase positive health outcomes. Even outside of the typical “healthcare” world, there are plenty of opportunities to encourage change, healthier food options in low-income areas, community gardens or even increased transportation resources.
The list could go on, but all of the above are specific actions that promote a healthy lifestyle. For example, by increasing the transportation resources in an area, individuals that might not have the ability to travel to health services now have the opportunity to take public transportation to get to their desired location.
Of course, it is possible to address health outcomes in the healthcare system. There have been several initiatives at the state and federal level to address SDoH, such as the Accountable Health Communities Model that addresses the gap between clinical care and community services. This innovative program focuses on the following:
- Screening of community-dwelling beneficiaries to identify unmet health-related social needs
- Referral of community-dwelling beneficiaries to increase awareness of community services
- Provision of navigation services to assist high-risk community-dwelling beneficiaries access community services
- Encouraging alignment between clinical and community services to ensure that community services are available and responsive to the needs of community-dwelling beneficiaries.
SDoH During the COVID-19 Public Health Emergency
COVID-19 disproportionately affected people of color. In an article published by The New York Times, data showed 23 COVID cases per 10,000 white individuals, compared to 62 and 73 COVID cases per 10,000 for black and Latino individuals, respectively. Some challenges were testing availability and education to ensure that individuals were aware of testing sites, how testing works, and what to do if their test is positive.
Quarantine requirements also posed a challenge for individuals who lived with others in joint households or shared housing facilities. These individuals were potentially risking the health of others, and it was important to identify ways in which these individuals could safely quarantine or isolate. An article published by The Washington Post, highlighted the success of several countries in curtailing the virus and preventing community spread. These countries provided government-sponsored facilities for individuals to safely quarantine following exposure. Federal governments should allocate funds to increase the number of facilities available, but also make them available to all individuals no matter the community they come from.
By sharing COVID-19 infection and mortality data by race and zip code, experts in the field were able to identify trends in the community, allowing them to provide more assistance such as increased testing, quarantine facilities, or treatment. Taking this a step further, collecting SDOH data in a shared database, accessible to various healthcare providers, can help providers better understand how the SDOH are impacting health. This data can be shared and used in precision medicine studies to better evaluate social and behavioral data and its effects on health equity on a much larger scale.
Improving SDoH Across US Communities
Implementing these changes can lead to improved health outcomes, but often need public funding and government support to come to fruition. It is important to ensure local and state representatives are aware of the changes necessary to keep our communities safe.
During the pandemic, there was legislation, such as the CARES Act, that provided fast and direct economic assistance for American workers, families and small businesses, to preserve jobs and protect American industries. In the future, we need to look to and encourage these policymakers to develop programs that can provide support to those communities that face the most hardship.
Wanting to reach out to your representatives? Find out who they are, here.
Sources:
Social Determinants of Health. (n.d.). Retrieved August 20, 2020, from https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-of-health
Hensrud, D. D. (2000). Clinical Preventive Medicine in Primary Care: Background and Practice: 1. Rationale and Current Preventive Practices. Mayo Clinic Proceedings, 75(2), 165-172. doi:10.4065/75.2.165
Accountable Health Communities Model. (n.d.). Retrieved August 20, 2020, from https://innovation.cms.gov/innovation-models/ahcm