This guest post is written by Patty Upham, RN, VP of Clinical Services for Health Recovery Solutions, and long-time nurse.
I have been a nurse for over 45 years and have witnessed the myriad challenges facing our front line nurses. The relentless COVID pandemic may have accelerated the national nursing shortage, but the problem and the underlying issues have been growing for some time. Only now, the impact is more deeply felt. So much so that the American Nurses Association (ANA) released a letter written to the Secretary of Health and Human Resources sounding the alarm.
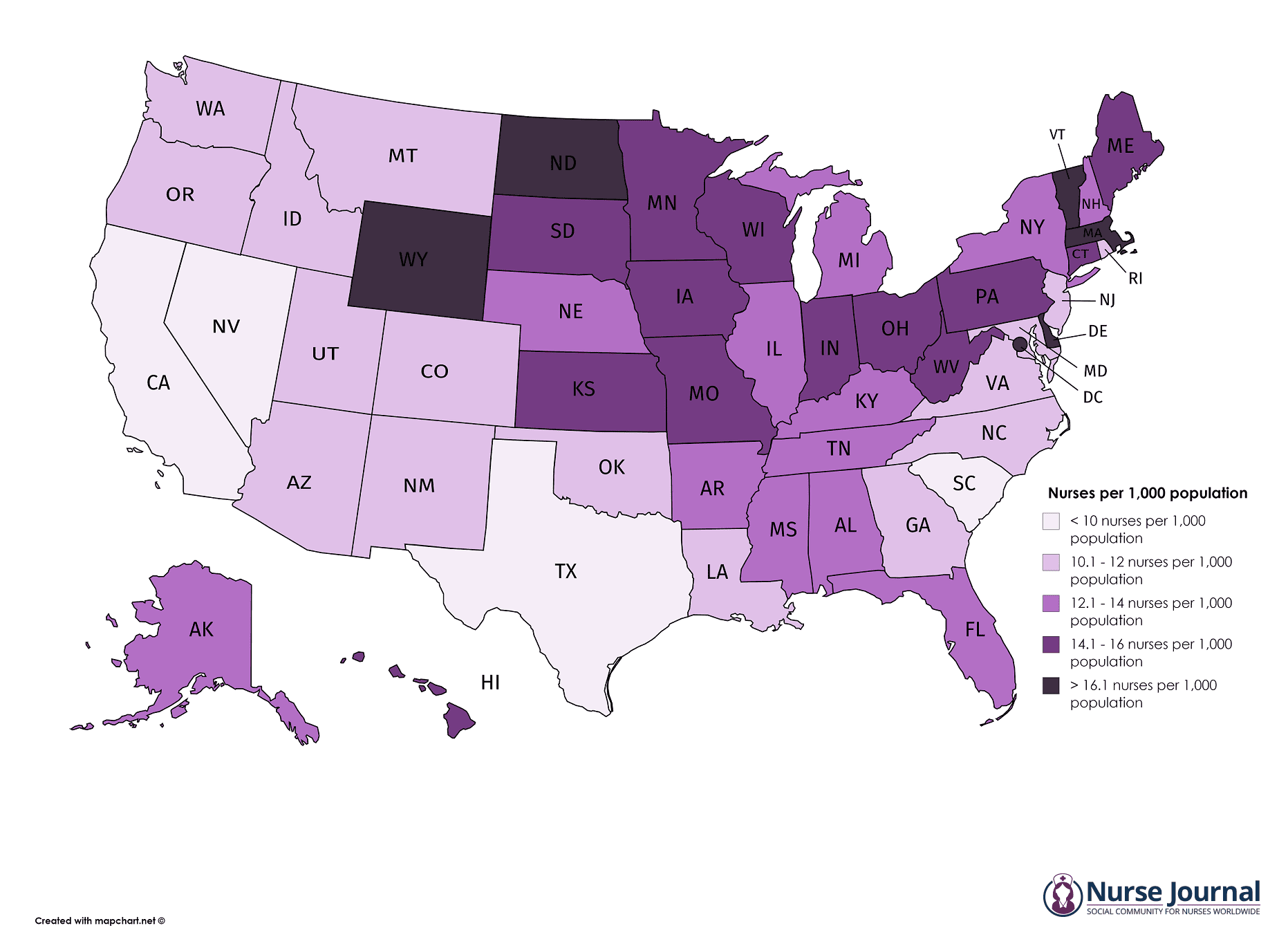
The Nursing Shortage Crisis, by the Numbers
From the American Nurses Association letter:
“Mississippi has reported that it has seen a decrease of 2,000 nurses since the beginning of 2021.
Hospitals in Tennessee are operating with 1,000 fewer staff than at the beginning of the pandemic, prompting them to call on their National Guard for reinforcement.
Texas is recruiting 2,500 nurses from outside the state, a number that will still fall short of expected demand.
Louisiana had over 6,000 unfilled nursing positions open across the state before the Delta variant caused a surge in cases. This shortage may become more acute as the state deals with the aftermath of Hurricane Ida.”
COVID’s Impact on the Nursing Crisis
The unparalleled strain the pandemic has caused for all of health care, has hit nurses particularly hard. Their role at the bedside puts them front and center to the chaos, grief and loss. Already a tough job, the demands of the care of COVID patients has been felt all across the health care landscape.
Overflowing emergency rooms, urgent cares, hospitals, home health and hospice agencies, the shortage impacts all sites of care, their staff and untold numbers of patients.
The real heart of the nursing shortage, now an emerging public health crisis, is the emotional, physical, economic and spiritual burden direct patient care nurses suffer. Mostly women, many single mothers, efforts to recruit and retain nurses must include addressing the particular issues women face; competitive wages commensurate with skill and experience, access to reliable and affordable child care, a better work life balance and a career path to promotion. These solutions lie in the future and will require a committed effort to change the current dynamic.
The problem at hand, however, is how do we do more with less now. Hospitals are limiting admissions, Emergency Rooms are turning away patients and Home Health and Hospice Agencies cannot take on new patients. The current state is a real emergency.
How Telehealth and Remote Patient Monitoring Can Help
HRS Virtual Care and Remote Patient Monitoring is a critical part of the immediate solution for the overburdened home health and hospice industry. And, by improving capacity in home based care, the burden can also be mitigated for hospitals and emergency departments.
HRS has developed a model of care: The HRS Virtual Visit Model that addresses the nursing shortage for patients cared for in the home - where more and more patients are being diverted to ease the burden on overcrowded and understaffed hospitals and emergency departments.
The HRS Virtual Visit Model mobilizes its virtual visit and RPM capabilities to increase the total number of patient encounters with their home care nurses while reducing in person nursing visits.
Virtual Care is now an accepted form of care by nurses, physicians and patients. The benefits are significant: less travel time for nurses; reduced cost of care delivery; more timely access to care; improved communication capability between nurses and patients with talk, text and video.
Reducing the number of in person home visits while still providing the same number or more actual encounters frees the front line nurse to do fewer in person patient visits while enabling them to take on more patients. Additional support to the front line team in this model includes the Telehealth Nurse who monitors the patient’s biometrics and symptom surveys as well as the Virtual Visit Nurse who connects with the patient remotely to support the plan of care, clinically assess and educate the patient. Coordination is key across the care team.
Developed by the HRS Clinical Team, the HRS Virtual Visit Model includes the strategy, metrics and tools to support the model launch. The ability to increase home based nursing capacity, accept more referrals in support of hospitals and health systems and deliver positive patient outcomes during a time of a national nursing shortage is the goal of HRS Virtual Visit Model.
CLIENT NEWS
Southcoast Health Reduces In-Home Care Costs and Hospital Readmissions
The Southcoast Health Visiting Nurse Association (VNA) saved an average of four in-home nursing visits annually, and generated over $500,000 in cost savings, while achieving a 7% 30-day readmission rate for 2,621 high-risk patients over the last 16 months leveraging HRS' remote patient monitoring (RPM) and virtual visit program.