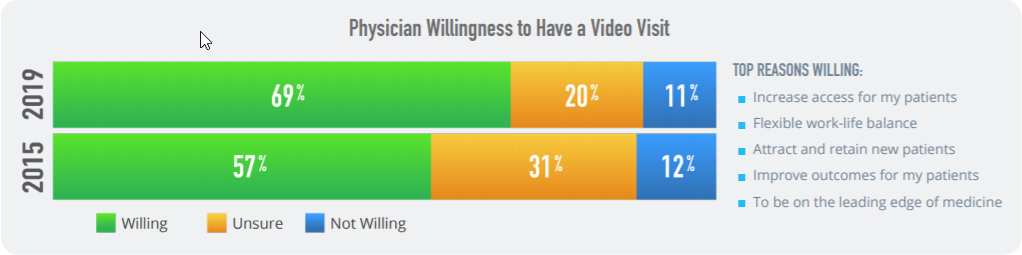
Fierce Healthcare recently reported a study revealing 67% of physicians indicated their willingness to incorporate telehealth into their patients' care plans, a nearly 10% increase from just three years prior. The rapid increase confirms clinicians' preference for telehealth into patient care.
The Center for Medicare and Medicaid Services’ (CMS) Next Generation ACO telehealth waiver allows for the expansion of telehealth implementation across the United States, regardless of geographic location. This article outlines the Next Gen ACO Model, the waiver, and the benefits they create. The Next Gen ACO telehealth waiver is one of several steps CMS has taken in the last year to broaden patient access to care via telehealth services.
What is a Next Generation ACO?
A Medicare ACO is a patient-centered organization of health care providers who coordinate and deliver high quality, lower-cost care to Medicare recipients. Both patients and providers benefit from ACO’s. Utilizing centralized patient medical records and history, clinicians can better coordinate care across a patient’s medical team, while patients maintain their providers and health benefits.
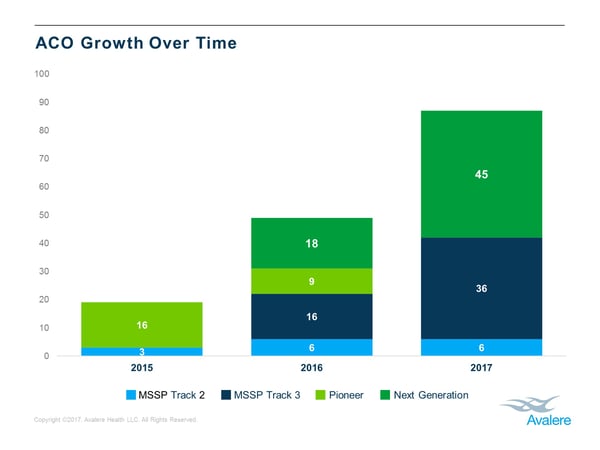
Medicare incentivizes ACOs to reduce costs while increasing care quality, allowing ACOs to retain a portion of the savings they achieve. A Next Generation ACO is the name given to any ACO participating in the Next Gen ACO Model created by CMS. Since its inception in 2016, participation in the program has grown from 18 ACOs to 41 ACO’s across 29 states in 2019.
ACOs are selected for participation by CMS based on comprehensive eligibility criteria including organizational structure, leadership and management, financial planning and risk-sharing experience, patient-centeredness, and clinical care model.
Once selected, the model allows for ACO’s to assume greater financial risks and rewards than are allowed under the Shared Savings Program (MSSP), the program by which non-Next Generation ACOs must abide. The Next Gen ACO model tests whether financial incentives paired with patient engagement and care management tools allow ACOs to improve patient outcomes and reduce costs compared to Medicare fee-for-service (FFS) beneficiaries.
Understanding the Telehealth Waiver
Telehealth waivers allow health care providers to use specific service codes to bill for telehealth services.
Prior to the Telehealth Waiver, patients could access telehealth in rural areas from healthcare providers that met CMS’ Health Professional Shortage Areas (HSPA) requirements. The Telehealth Waiver expands patient access further, no longer requiring Next Gen ACOs to meet HSPA restrictions.
The waiver expands “originating sites” for telehealth, covering the following locations for patients to receive telehealth services: physician or practitioner offices, hospitals, clinics and federally qualified health centers, hospital-based renal dialysis centers, skilled nursing facilities, and community mental health centers. In addition to the listed sites, the waiver enables a patient’s home to be considered an “originating site” for telehealth services, a vital step in empowering patients to stay in their home, while providing constant support.
 Impact on the Population
Impact on the Population
Next Gen ACOs and the telehealth waiver provide an opportunity for patients to overcome existing barriers to healthcare, allowing some of the 51% of adults living with a chronic disease in America to access the quality care they depend upon. Some ways in which the waiver is being employed to provide maximum benefits include:
-
-
Integrating telehealth with existing patient health records to determine high-risk patients.
-
Expanding post-acute services to monitor factors like medication non-adherence.
-
In using the waiver in the ways listed above, telehealth programs offered through Next Gen ACOs provide care at a reduced cost to all parties: the state, the provider, and the patient. States see savings benefits through reduced cost of care, while financial incentives to provide telehealth monitoring for patients allow healthcare providers to incur savings as well.
Telehealth allows patients to receive prompt, high-quality, coordinated care while maintaining independence through self-monitoring and reporting - contributing further to cost savings through reduced travel time and expense. Telehealth provides many benefits for the millions of Americans living with chronic disease, and the Next Gen ACOs and telehealth waiver expands those benefits to provide necessary care to patients regardless of location.
References:
Fierce Healthcare. (2019, April 15). 1 in 5 Physicians use Telehealth. Burnout may Drive more Adoption, Survey Says. Retrieved from https://www.fiercehealthcare.com/tech/22-physicians-use-telehealth-and-burnout-may-drive-more-adoption-survey
National Conference of State Legislatures. (n.d.). Chronic Disease Prevention and Management. Retrieved from http://www.ncsl.org/documents/health/chronicdtk13.pdf
Next Generation ACO Model. (n.d.). Retrieved from https://innovation.cms.gov/initiatives/Next-Generation-ACO-Model/
Next Generation ACO Model - Fact Sheet. (n.d.). Retrieved from https://innovation.cms.gov/Files/fact-sheet/nextgenaco-fs.pdf
Next Generation ACO Model Frequently Asked Questions. (n.d.). Retrieved from https://innovation.cms.gov/Files/x/nextgenacofaq.pdf